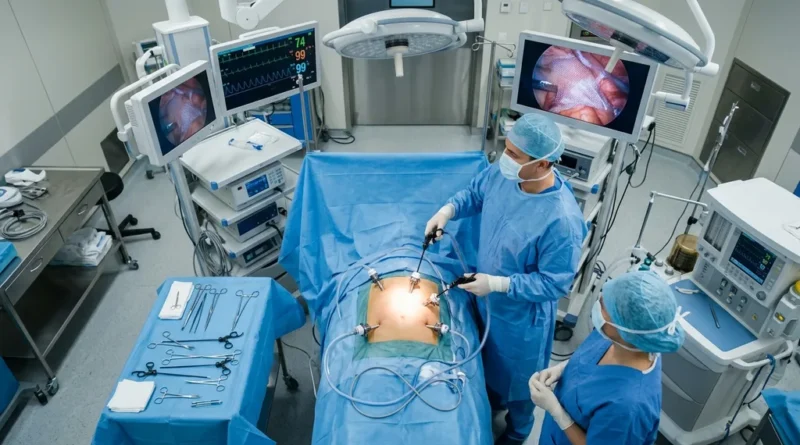
Types of Hernia Repair Surgery: Laparoscopic, Open, and More
What Is a Hernia?
A hernia occurs when an organ or tissue pushes through a weak spot in the surrounding muscle or connective tissue. In the abdomen, this means internal contents — usually part of the intestine — protrude through a tear in the abdominal wall. Hernias most commonly occur in the groin, abdomen, belly button, and upper thigh.
Hernias rarely resolve on their own. Most worsen gradually, and the primary risk is strangulation — where the herniated tissue becomes trapped and loses its blood supply, a surgical emergency. According to the Mayo Clinic, surgery is the standard treatment for symptomatic hernias in most patients.
Types of Hernias
Hernias are classified by location:
- Inguinal hernia: The most common type in men. Occurs in the inner groin when intestinal tissue pushes through the inguinal canal.
- Umbilical hernia: Near the belly button. Common in newborns and women who have had multiple pregnancies.
- Epigastric hernia: Between the belly button and breastbone. More common in infants due to underdeveloped abdominal walls.
- Spigelian hernia: Along the edge of the rectus abdominis muscle. Rarer and harder to detect because it sits below the skin surface.
- Incisional hernia: Develops at the site of a previous abdominal surgery incision. More common in older or overweight patients.
- Diastasis recti: Weakening of the midline between the rectus abdominis muscles, creating an epigastric bulge without a true hernia sac.
How Surgeons Decide Which Repair to Use
Hernia repair is one of the most common surgical procedures worldwide. A 2016 systematic review in the World Journal of Surgery found that abdominal wall hernias affect approximately 1.7% of all adults and up to 4% of those over age 45. The choice of repair depends on hernia type and size, patient health and age, prior surgeries, and surgeon experience.
Laparoscopic Hernia Repair
Laparoscopic repair is now the most widely performed hernia surgery. The surgeon makes two or three small incisions (under 1 cm each), inserts a laparoscope — a thin camera — and uses specialized instruments to repair the hernia from the inside. The abdomen is inflated with CO2 to create working space. A synthetic mesh is typically placed over the defect to reinforce it.
Advantages of laparoscopic repair
- Smaller incisions produce less scarring
- Shorter hospital stay — often same-day discharge
- Less post-operative pain than open surgery
- Faster return to normal activities (1–2 weeks for light activity)
- Lower risk of wound infection
- Recurrence rates comparable to open surgery
When it is not the best choice
Laparoscopic repair requires general anesthesia. It is not ideal for patients who cannot tolerate that, or for very large or complex hernias that need direct visualization. Robotic-assisted laparoscopy is an emerging variation that offers even greater precision in complex cases.
Open Hernia Repair
Open repair has been performed for over a century and remains the standard for large, complex, or recurrent hernias. The surgeon makes a single larger incision directly over the hernia, pushes the tissue back into place, and reinforces the abdominal wall with mesh or sutured tissue.
Advantages of open repair
- Suitable for large, bilateral, or recurrent hernias
- Can be performed under local or spinal anesthesia in select patients
- Direct access and visibility for complex anatomies
- Long track record with well-established outcomes data
Trade-offs
Open surgery results in a larger scar and typically involves 4–6 weeks of recovery before returning to heavy activity. Scar tissue from prior open repairs can complicate future minimally invasive procedures, so the choice of initial approach matters for patients likely to need future abdominal surgery.
Reconstructive Surgery for Complex Hernias
Abdominal wall reconstruction is reserved for the most complex cases: large incisional hernias, recurrent hernias after prior repair, or hernias with significant muscle loss. The procedure restores both the structural integrity and function of the abdominal wall, often using a technique called component separation to bring the muscle edges back together across a wide defect.
Advantages
- Addresses hernias that simpler methods cannot adequately repair
- Treats open abdominal wounds and reinforces muscular integrity
- Can restore near-normal abdominal wall function in patients with severe defects
Considerations
Reconstructive surgery is more invasive and carries higher risks of infection, blood loss, and post-operative discomfort than laparoscopic or standard open repair. It is typically performed by specialist hernia surgeons at academic or tertiary care centers. Recovery is longer, and patients need realistic expectations about the process. If you are navigating a complex surgical recovery, understanding structured post-operative care — similar to what medically supervised recovery programs provide — makes a significant difference in outcomes.
Mesh in Hernia Repair
Surgical mesh is used in the majority of adult hernia repairs regardless of the surgical approach. It provides reinforcement over the repaired defect, reducing the chance the hernia will recur. Mesh is available in synthetic materials (polypropylene, polyester) and biologic options derived from human or animal tissue.
Mesh repair reduces hernia recurrence rates to low single digits — significantly lower than the 10–30% recurrence seen with suture-only repairs. The current consensus in surgical guidelines treats mesh as the gold standard for adult hernia repair except in specific circumstances, such as infected fields where biologic mesh may be preferred, or pediatric cases where primary tissue repair is standard.
Frequently Asked Questions
Do all hernias need surgery?
Most hernias worsen over time and do not heal on their own. Small, painless hernias in low-risk patients may be monitored with watchful waiting, but surgery is generally recommended to prevent complications like strangulation, where the herniated tissue loses its blood supply — a potentially life-threatening emergency.
Which is better — laparoscopic or open hernia surgery?
Both approaches are effective with comparable long-term outcomes. Laparoscopic surgery generally produces less post-operative pain, smaller scars, and faster recovery. Open surgery is preferred for very large hernias, complex cases, or patients who cannot tolerate general anesthesia.
Is mesh always required for hernia repair?
Mesh is the current gold standard for adult hernia repair because it reduces recurrence rates to low single digits. Non-mesh repairs are generally reserved for children or specific adult cases where mesh is contraindicated — such as in infected surgical fields.
How long does hernia repair recovery take?
Laparoscopic and robotic surgery patients can typically return to light activities in 1–2 weeks. Open surgery patients usually need 4–6 weeks before resuming heavy activity. Heavy lifting is restricted for several weeks regardless of technique to allow the repair to fully consolidate.
Can a hernia come back after surgery?
Yes, recurrence is possible. Mesh repair reduces this risk to low single digits, but smoking, obesity, and straining during recovery all increase recurrence probability. Patients with recurring hernias are typically candidates for reconstructive abdominal wall surgery.